

Respiratory System
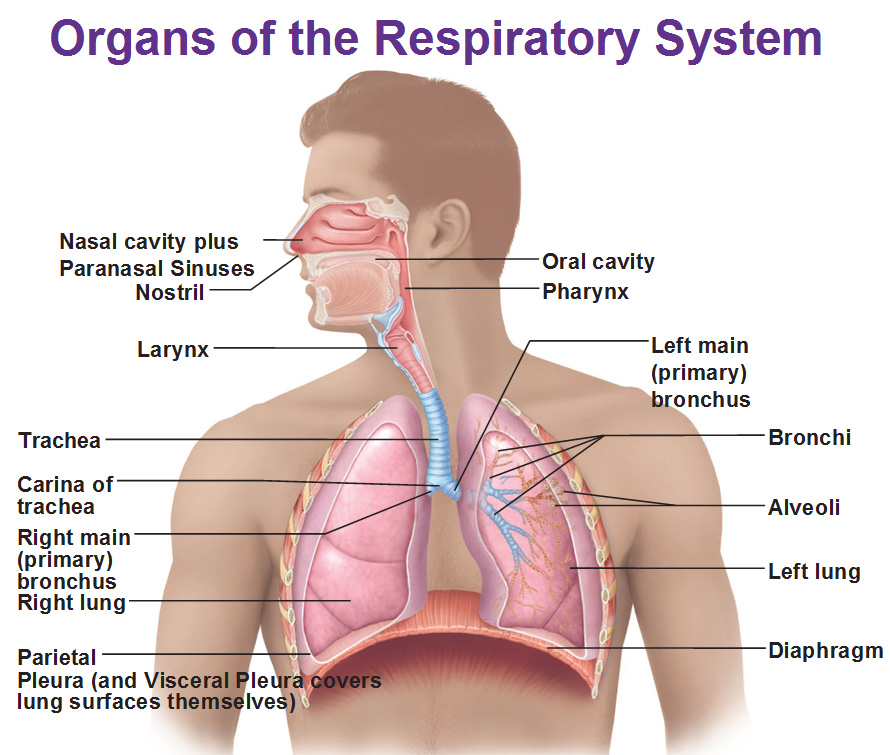
The respiratory system is responsible for gas exchange—bringing oxygen into the body and removing carbon dioxide. Air enters through the nasal cavity, passes through the pharynx and larynx, then travels down the trachea. The trachea divides into two main bronchi (left and right), which further branch into smaller bronchioles within the lungs. At the end of the bronchioles are tiny air sacs called alveoli, where oxygen diffuses into the bloodstream and carbon dioxide moves out.
In febrile respiratory illnesses, inflammation can affect any part of this pathway, from the nasal passages (rhinitis) to the alveoli (pneumonia). Fever often accompanies these conditions as part of the body's immune response.
Diagnostic Scope
This module analyzes febrile patterns in conjunction with respiratory symptoms. By correlating body temperature fluctuations with cough, fatigue, and shortness of breath, the AI identifies potential viral or bacterial pulmonary infections.
Common Febrile Respiratory Conditions
Influenza
Characterized by sudden onset of high fever, muscle aches, dry cough, and fatigue. Typically seasonal, caused by influenza A or B viruses.
COVID‑19
Fever, cough, and shortness of breath are hallmarks. Loss of taste or smell may also occur. Caused by SARS‑CoV‑2, with varying severity.
Pneumonia
Infection of the lung parenchyma. Presents with fever, productive cough, pleuritic chest pain, and sometimes confusion in older adults.
Bronchitis
Inflammation of the bronchial tubes. Often follows a cold; fever may be low‑grade, with persistent cough and mucus production.
Who Is at Higher Risk?
While anyone can develop a febrile respiratory illness, certain factors increase susceptibility and the likelihood of severe disease.
Age
- Young children (under 5) and older adults (over 65) are more vulnerable.
- Infants have immature immune systems.
- Older adults often have weakened immune responses and chronic conditions.
Underlying conditions
- Chronic lung disease (asthma, COPD).
- Heart disease, diabetes, kidney disease.
- Immunocompromised states (HIV, chemotherapy, transplant recipients).
Lifestyle & environment
- Smoking or exposure to secondhand smoke.
- Crowded living conditions (dorms, nursing homes).
- Occupational exposure (healthcare workers, first responders).
Reducing Your Risk
Vaccination and simple hygiene measures are the most effective ways to prevent respiratory infections.
- Get vaccinated. Annual flu shots and COVID‑19 boosters reduce the chance of severe illness.
- Wash hands frequently with soap and water, or use alcohol‑based hand sanitizer.
- Avoid close contact with people who are sick.
- Cover coughs and sneezes with a tissue or your elbow.
- Wear a mask in crowded indoor settings during respiratory virus season.
- Stay home when ill to prevent spreading infection.
Recent Advances in Respiratory Medicine
Rapid molecular testing
Point‑of‑care PCR tests can now identify influenza, RSV, and COVID‑19 in under 30 minutes, allowing earlier antiviral treatment.
Novel antivirals
New drugs like baloxavir for influenza and nirmatrelvir/ritonavir for COVID‑19 shorten illness duration and reduce hospitalization risk.
AI‑assisted chest imaging
Deep learning algorithms can detect pneumonia and COVID‑19 patterns on chest X‑rays with accuracy comparable to expert radiologists.
When to seek further evaluation: Persistent fever lasting more than three days, worsening shortness of breath, chest pain, or confusion require immediate medical attention. Pulse oximetry readings below 92% while breathing room air also warrant urgent care.