

Arterial System and Blood Pressure
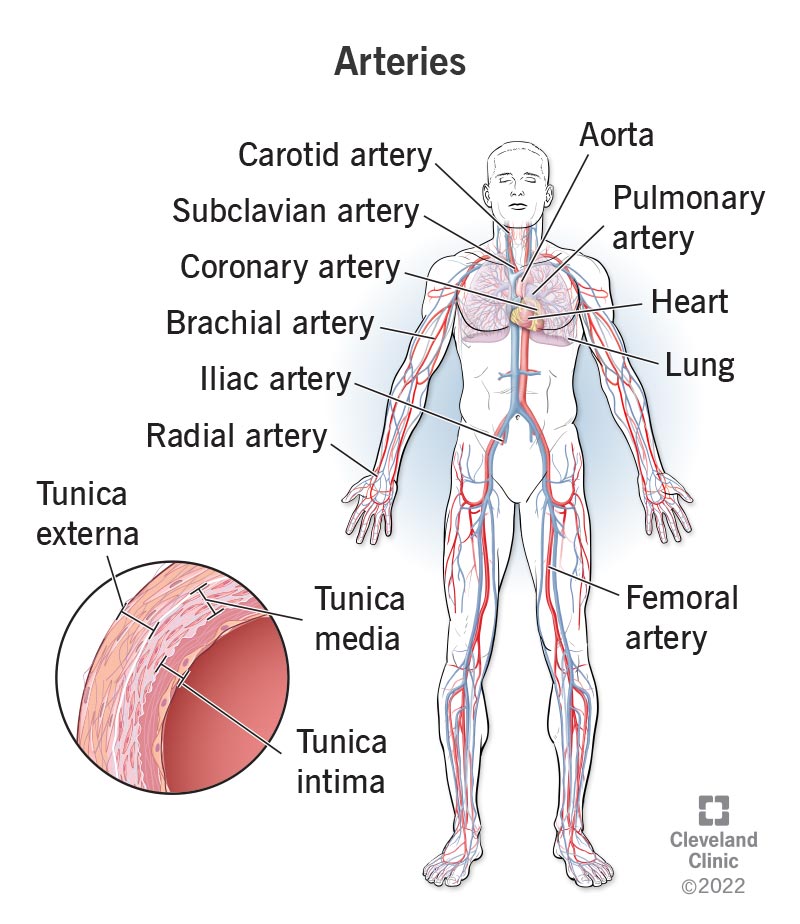
Blood pressure is the force exerted by circulating blood against the walls of the arteries. It is determined by two factors: the amount of blood the heart pumps per minute (cardiac output) and the resistance to flow in the arterioles (peripheral vascular resistance). Systolic pressure represents the peak pressure during heart contraction, while diastolic pressure is the lowest pressure when the heart relaxes between beats.
Chronic elevation of pressure—hypertension—forces the heart to work harder and can damage the delicate endothelial lining of arteries. Over time, this contributes to atherosclerosis, weakening of vessel walls, and increased risk of stroke, heart attack, and kidney disease.
Diagnostic Scope
Hypertension evaluation involves the multi-dimensional analysis of high-pressure load on arterial walls. The system categorizes readings into Elevated, Stage 1, or Stage 2 Hypertension, assessing the risk of secondary complications like renal strain or cerebrovascular events.
Blood Pressure Categories
Normal
Systolic less than 120 mmHg and diastolic less than 80 mmHg. Optimal for cardiovascular health.
Elevated
Systolic 120–129 mmHg and diastolic less than 80 mmHg. Indicates increased risk of progressing to hypertension.
Stage 1 Hypertension
Systolic 130–139 mmHg or diastolic 80–89 mmHg. Lifestyle changes and often medication are recommended.
Stage 2 Hypertension
Systolic ≥140 mmHg or diastolic ≥90 mmHg. Requires prompt treatment with medication and lifestyle modifications.
Hypertensive Crisis
Systolic >180 mmHg and/or diastolic >120 mmHg. Emergency care needed.
What Leads to Hypertension?
The causes of high blood pressure are often multifactorial. Identifying risk factors helps guide prevention and treatment.
Modifiable factors
- Unhealthy diet high in sodium and low in potassium.
- Physical inactivity and sedentary lifestyle.
- Excess body weight or obesity.
- Tobacco use and excessive alcohol intake.
- Chronic stress and poor sleep.
Non‑modifiable factors
- Age (risk increases with age).
- Family history of hypertension.
- Race (more common in African‑descent individuals).
- Chronic kidney disease.
Secondary causes
- Kidney disease (renovascular hypertension).
- Adrenal tumors (e.g., pheochromocytoma).
- Thyroid disorders.
- Obstructive sleep apnea.
- Certain medications (NSAIDs, steroids, decongestants).
Controlling Blood Pressure
Lifestyle changes are the foundation of hypertension prevention and management, often complementing medication.
- Reduce sodium intake. Aim for less than 2,300 mg per day (ideally 1,500 mg for greater benefit).
- Adopt the DASH diet. Emphasize fruits, vegetables, whole grains, low‑fat dairy, and lean protein.
- Exercise regularly. At least 150 minutes of moderate aerobic activity per week.
- Maintain a healthy weight. Losing even 5‑10 pounds can lower blood pressure.
- Limit alcohol. No more than one drink per day for women, two for men.
- Quit smoking. Each cigarette causes a temporary spike in pressure and damages arteries.
- Monitor at home. Regular self‑measurement helps track progress and alert to changes.
Recent Advances in Hypertension Care
Renal denervation
A catheter‑based procedure that disrupts overactive renal nerves, reducing blood pressure in patients resistant to multiple medications.
Ultra‑long‑acting therapies
New drug formulations (e.g., subcutaneous injections every 6 months) are being studied to improve adherence in poorly controlled hypertension.
Artificial intelligence in BP monitoring
Wearable devices with AI algorithms can now provide continuous, cuff‑less blood pressure estimation, enabling early detection of nocturnal hypertension.
When to seek further evaluation: If your home readings are consistently above 135/85 mmHg, or if you experience symptoms like severe headache, blurred vision, chest pain, or shortness of breath, consult a healthcare provider promptly. Ambulatory blood pressure monitoring may be recommended to confirm the diagnosis.